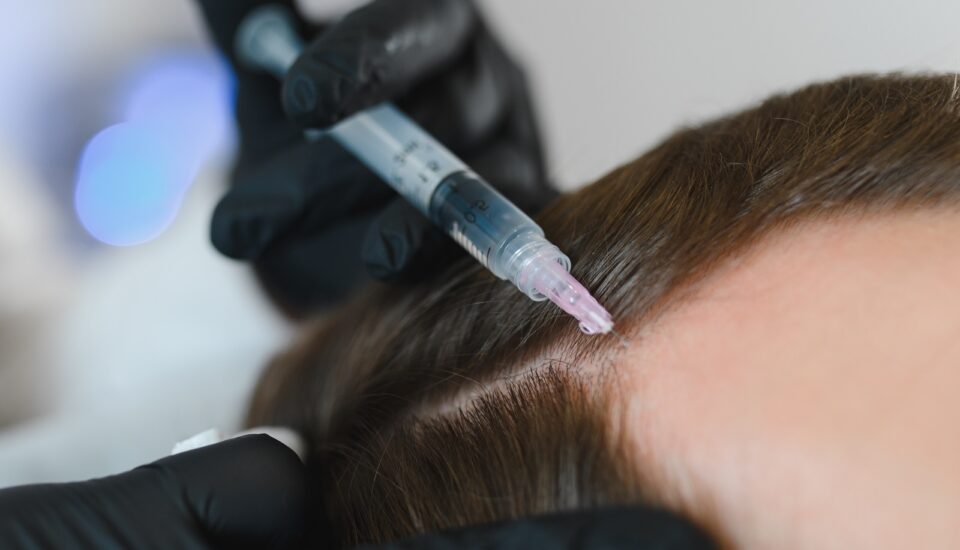
What Is PRP?
PRP involves concentrating a patient’s own platelets and growth factors from peripheral blood and injecting them into the scalp. These growth factors can influence:
- Cellular signalling within the hair follicle
- Local vascular supply and nutrient delivery
- Inflammatory balance within the scalp environment
PRP acts primarily as a biological activation signal. It does not create new hair follicles and does not alter genetic susceptibility to hair loss.
How PRP Works — and Why It Has Limits
PRP provides signalling that may stimulate follicles that are still biologically viable.
Using a practical analogy, the hair follicle can be viewed as a factory. Genetic programming sets production limits, while PRP acts as a stimulus — comparable to improving logistics and signalling to encourage activity.
However, stimulation alone is insufficient if the factory lacks resources.
PRP cannot:
- Create new hair follicles
- Reverse advanced genetic hair loss
- Compensate for significant nutritional deficiencies
- Restore impaired mitochondrial or ATP production
- Overcome systemic inflammation, oxidative stress, or hormonal disruption
When PRP May Be Helpful
PRP may be considered when:
- Hair loss is early or moderate
- Follicles are miniaturising but still active
- Diffuse thinning is present
- Used to support healing or native hair after transplantation
- Combined with appropriate systemic optimisation
PRP should be viewed as adjunctive, not standalone, therapy.
When PRP Is Unlikely to Be Effective
PRP is generally less effective when:
- Hair loss is advanced or long-standing
- Follicles are no longer viable
- Donor and recipient density are poor
- Systemic contributors remain unaddressed
- Expectations exceed biological limits
In these situations, PRP may add cost without meaningful benefit.
PRP Protocol Quality Matters
Outcomes depend heavily on protocol quality, including:
- Blood volume collected
- Platelet concentration achieved
- Processing technique
- Size of the treatment area
Small blood volumes may be adequate for limited areas but are often insufficient for larger regions such as the frontal scalp or crown.
Combining PRP With Other Treatments
When clinically appropriate, PRP may be combined with:
- Microneedling
- Medical therapies
- Nutritional and metabolic optimisation
Combination strategies should be individualised following assessment.
Frequently Asked Questions
Q1 :Does PRP regrow lost hair?
Any benefit is typically temporary and requires maintenance sessions.
Q2 :Is PRP an alternative to hair transplantation?
No. PRP does not replace surgery in advanced hair loss.
Q3 :Can PRP worsen hair loss?
PRP does not worsen hair loss. Limited results usually reflect disease progression rather than harm.
Q4 :Is PRP suitable for everyone?
No. PRP should be offered selectively after physician-led assessment.
Q4 :Is PRP suitable for everyone?
No. PRP does not regrow hair where follicles are absent. It may improve thickness or slow loss in viable follicles.
Considering PRP?
A structured medical consultation can help determine whether PRP is appropriate and whether systemic optimisation should be addressed first.