The Consultation Pathway
A successful hair restoration outcome begins with a structured consultation pathway. This ensures that diagnosis, expectations, and treatment decisions are aligned before any procedure is considered.
Our consultation pathway typically includes:
Initial assessment to understand the pattern, severity, and stability of hair loss
- Discussion of medical history, lifestyle factors, and previous treatments
- Evaluation of donor availability and long‑term feasibility
- Explanation of all appropriate options — including the option of no treatment
- Clear discussion of expected outcomes, limitations, risks, and timelines
This stepwise approach reduces the risk of inappropriate treatment and is a key reason why experience matters in hair restoration.
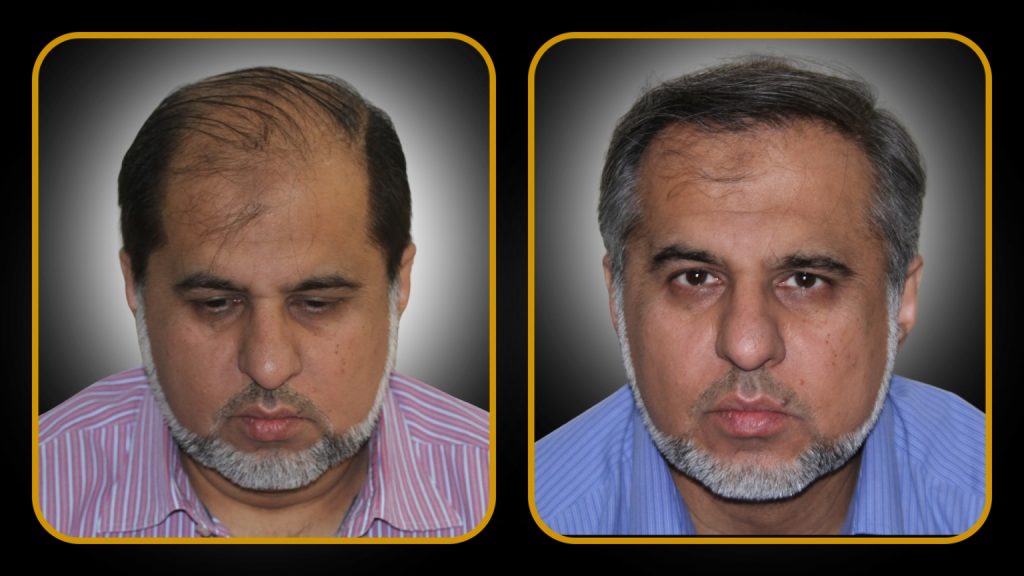
Hair Transplant Results
We provide a structured, step‑by‑step pathway for men and women with hair loss — ranging from diagnosis and medical optimisation to hair transplantation in carefully selected candidates.





What We Do
We provide a structured, step‑by‑step pathway for men and women with hair loss — ranging from diagnosis and medical optimisation to hair transplantation in carefully selected candidates.
Step 1: Medical Evaluation (Root‑Cause Assessment)
Every plan begins with understanding why hair loss is occurring.
This may include:
- Detailed history (onset, triggers, pattern change, shedding vs thinning)
- Scalp and hair examination (including scarring vs non‑scarring patterns)
- Review of medications, supplements, and relevant medical conditions
- Assessment of progression risk and long‑term trajectory
- Targeted laboratory tests only when clinically relevant (for example iron status, thyroid markers, vitamin status, hormones, metabolic markers)
Not every patient needs blood tests. Testing is used to avoid guessing — not as a routine or a sales tool.
Step 2: Restorative Planning (Long‑Term Strategy)
Hair restoration must be planned over years, not months.
Planning includes:
- Anticipating future hair loss progression
- Preserving donor reserves for long‑term durability
- Assessing healing capacity and systemic health
- Clear discussion of limitations, trade‑offs, and timelines
This is where many poor outcomes originate: short‑term thinking applied to a progressive biological condition.
Tools We May Use (When Appropriately Indicated)
Not all patients need all treatments. Some need none.
Depending on diagnosis and suitability, tools may include:
- Medical therapy (when evidence‑based and appropriate)
- Nutrient and metabolic optimisation
- Scalp and inflammatory control
- Regenerative adjuncts in selected cases
- Hair transplantation in suitable candidates
Mandatory clarity:
- Not every hair‑loss pattern is suitable for surgery
- Some conditions require medical stabilisation first
- Some do not benefit from transplantation at all
If a procedure is unlikely to help, we will say so.
Functional Medicine Perspective (The Whole‑Body Context)
Hair follicles are metabolically active structures. Their ability to respond to treatment depends on the internal biological environment.
A functional medicine approach recognises that hair loss is often not a single‑factor problem and cannot be managed simply by selecting a procedure such as PRP, exosomes, or transplantation.
We therefore consider:
- Nutrient availability and absorption
- Inflammation and oxidative stress
- Insulin resistance and metabolic health
- Stress physiology and cortisol burden
- Thyroid and sex hormone balance
Functional medicine does not replace conventional medical or surgical care. Instead, it provides the biological context that explains why outcomes vary and why some patients require stabilisation or optimisation before any procedure is appropriate.
Hair Transplantation (When Indicated)
Hair transplantation is a powerful surgical tool, but it requires a high level of expertise to be performed safely and responsibly.
Surgery is considered only when:
- The pattern of hair loss is predictable
- There is a good match between donor‑hair availability and present/future recipient needs
- Donor reserves are adequate
- Expectations are realistic
- Long‑term planning is feasible
Surgical planning prioritises:
- Natural hairline design and facial framing
- Conservative and strategic use of grafts
- Transplantation to the crown as a lower priority in most younger patients
- Appropriate density‑to‑area balance
- Preservation of donor reserves for future needs
Complications and the Importance of Expertise
Hair transplantation is generally safe in experienced hands, but complications can never be eliminated entirely.
Potential risks include:
- Poor or uneven growth
- Shock loss of existing hair
- Scarring or donor overharvesting
- Unnatural hairline design or density
- Need for repair surgery
Experience significantly reduces these risks through proper case selection, conservative planning, and refined surgical technique. Many complications arise not from the procedure itself, but from poor judgement or overly aggressive treatment decisions.
Aggressive or poorly planned surgery may look impressive short‑term — and fail long‑term.
Situations That Require Caution or a Different Plan
Some scenarios require medical management, delay, or avoidance of surgery:
- Active inflammatory or scarring alopecia (must be stabilised first)
- Diffuse or unstable hair loss without a reliable donor pattern
- Significant metabolic disease or deficiencies impairing healing
- Expectations that exceed biological limits
In such cases, restraint is a medical decision — not a refusal of care.
Clinical Scope
Hair‑Loss Conditions Commonly Assessed
- Androgenetic hair loss (male and female pattern)
- Telogen effluvium (stress, illness, postpartum, nutritional drivers)
- Alopecia areata (requires medical diagnosis and monitoring)
- Scalp inflammation (seborrhoeic dermatitis, folliculitis, irritation)
- Scarring alopecia (only after specialist assessment and stabilisation)
What Defines a Physician‑Led Standard
- Diagnosis before procedure
- Long‑term planning rather than short‑term cosmetic fixes
- Donor preservation as a non‑negotiable principle
- Honest candidacy and refusal when appropriate
- Integration of medical, surgical, and biological considerations
Experience matters most when deciding what not to do.
Frequently asked Questions
Sometimes salon equipment requires professional setup—like installing styling stations or mirrors. A trained specialist can ensure everything is securely placed and fully functional for daily use.
Q1 :Do I need blood tests for hair loss?
Not always. Many patterns are diagnosed clinically. Targeted tests are used when history or examination suggests systemic contributors.
Q2 :Can stress cause hair loss?
Yes. Physical or psychological stress can trigger shedding (telogen effluvium). The goal is to identify triggers, support recovery, and rule out additional causes.
Q3 :Is hair transplantation permanent?
Transplanted hair is generally more resistant to androgen‑driven loss, but it is not immune to biology. Long‑term outcomes depend on diagnosis, planning, donor management, and whether ongoing hair loss is addressed.
Q4 :Why is the crown treated conservatively in younger patients?
The crown often continues to thin over time and requires many grafts for meaningful density. Early aggressive treatment can compromise long‑term results.
Q5 :Can women undergo hair transplantation?
Some women are suitable candidates, but careful evaluation is essential. Diffuse thinning patterns may not benefit from surgery.
Q6 :Is PRP or regenerative therapy enough on its own?
Sometimes helpful as an adjunct — but never a substitute for diagnosis, medical stabilisation, or appropriate surgical planning.
Sometimes helpful as an adjunct — but never a substitute for diagnosis, medical stabilisation, or appropriate surgical planning.


